Vein Clinic:
‑ Ultrasound Evaluation‑ Sclerotherapy
‑ Mini‑Phlebectomy
‑ Endovenous Laser Therapy
Our Vein Clinic is a state-of-the-art facility providing the latest technological advances in vein treatment, specializing in Endovenous Laser Therapy.
More info...
Gastro-esophageal Reflux
Occasional ingestion is common among adults - up to 25% of the world population requires over-the-counter antacids on a monthly basis. Half of those people experience daily heartburn while some experience regular heartburn that is not easily treated by non-prescription medicines. The symptoms experienced include a burning discomfort beneath the breast bone, caustic fluid in the throat, and indigestion after meals. These symptoms are typical of gastroesophageal reflux disease (GERD).
When swallowing food, a valve (also called “sphincter”) at the bottom of the esophagus prevents the backwash or reflux of stomach contents and acid back into the esophagus. Gastoesophageal reflux occurs when the lower sphincter is weak, letting the contents of the stomach backwash into the esophagus, making people experience heartburn. Certain foods may weaken the lower sphincter, making reflux worse. These include: caffeine, alcohol, chocolate, peppermint and fatty foods. Cigarette smoking also weakens the sphincter. As well, reflux is made worse by anything that increases pressure on the abdomen, such as straining, coughing, lifting, obesity, and pregnancy, which force stomach juices backwards against the valve.
Long-term exposure of the lower part of the esophagus to stomach acid can lead to major complications. The esophagus becomes inflamed which can lead to ulcers as well as bleeding. Inflammation of the esophagus can cause scarring, leading to narrowing of the esophagus and stricture formation, causing great difficulty swallowing food or even liquids. Some GERD patients regurgitate stomach juices all the way up the throat (usually at night), which can lead to caustic irritation of the voice box and wind pipe, causing some forms of asthma and chronic bronchitis. Severe damage to the lining of the esophagus by acid and bile can produce Barrett’s esophagus. Barrett’s esophagus is a change in the normal lining of the esophagus, generally after years of severe reflux problems. Patients with Barrett’s esophagus require a very close follow-up using endoscopy and biopsy to observe a possible progression to a more dangerous form of Barrett’s esophagus, which can lead to a dangerous form of cancer of the esophagus.
Lifestyle changes can help to improve reflux symptoms. Particularly, significant weight loss can dramatically help. Changing the daily diet to exclude foods that worsen the symptoms of GERD will help reduce symptoms. Similarly, quitting smoking will significantly reduce symptoms. Eating at least two hours before bedtime will reduce nighttime reflux and help patients get a good night‘s sleep. Elevating the head from the bed on six inch blocks will also improve nighttime reflux by letting gravity pull stomach juices away from the esophagus. Finally, regular use of antacids can neutralize the acid in the stomach, strengthening the valve and improving heartburn.
When symptoms appear to be unaffected by lifestyle changes, patients can be prescribed effective medicines to deal with reflux. Drugs called H2 blockers (Ranithidine) are used to reduce acid production by the stomach. If these medications are ineffective, a more powerful class of drugs called proton pump inhibitors (Losec, Pantoloc, Nexium or Prevacid) can be used which shut off acid production completely. Another group of drugs that can be used makes the stomach empty faster, thus pulling the stomach contents away from the esophagus.
 A small number of patients with GERD will continue having significant symptoms in spite of treatment with medications. Other patients are unable to afford the expense of prescription medications or are unable or unwilling to take medications regularly for the rest of their lives. For those patients surgery may be considered.
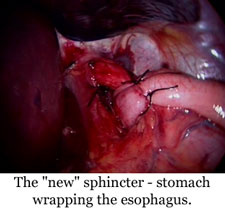
A small number of patients with GERD will continue having significant symptoms in spite of treatment with medications. Other patients are unable to afford the expense of prescription medications or are unable or unwilling to take medications regularly for the rest of their lives. For those patients surgery may be considered.We recommend the modern surgical treatment of GERD which involves a minimally invasive procedure. The most common operation is the laparoscopic Nissen fundoplication.. Five small 0.5 cm punctures are used to insert a tiny television camera and miniaturized instruments into the abdominal cavity. Essentially, a new sphincter is made by wrapping a small portion of the stomach around the lowest part of the esophagus. Studies indicate that over 90% of patients become symptom free and require no medications after the surgery.
Some patients may experience short-term side effects from the minimally invasive surgery. About 1 in 10 patients will experience the feeling of food sticking when swallowing. If this happens, it will last approximately 2-4 weeks and then gradually go away. Many patients will feel bloated after eating, this is generally a transient problem and this sensation improves with over the counter Simethicone products. If the proper dietary recommendations are followed, these symptoms are usually mild and improve after several weeks. However, flatulence and inability to eat large meals for a few weeks following surgery are common side effects.
Most patients rid of reflux symptoms and return to a normal lifestyle, eating all foods and requiring no medications after a laparoscopic Nissen fundoplication surgery. The average hospital stay is 1 or 2 nights. We recommend staying on full liquid diet for three weeks after the operation. After that solids can be gradually introduced into the diet.
You should notify your surgeon or your family doctor if the following appear:
- Lasting fever over 39°C, chills, increasing abdominal swelling, pain that in not relieved by the medications, inability to drink or eat, persistent nausea or vomiting, persistent cough or shortness of breath, purulent drainage (pus) from any incision, redness surrounding any of your incisions that is worsening or getting bigger.
Back to Minimally Invasive Surgery main page.
Contact Us
Minimally Invasive Surgery:
‑ Appendix‑ Bowel
‑ Gallbladder
‑ Gastro‑esophageal Reflux
‑ Hernias
‑ Rectum & Anus
‑ Spleen
‑ Varicose Veins
Endoscopy:
‑ Gastroscopy‑ Colonoscopy
Other:
‑ Breast‑ Thyroid